
Equal but Not the Same—2021 Update on Influenza Vaccines
As COVID-19 vaccination efforts continue, it is more important than ever for pharmacists to be equipped with the knowledge and resources to bust the myths surrounding vaccinations, particularly in preparation for the upcoming influenza season, which is expected to occur from October 2021 to May 2022.1 Infection can be caused by both A and B strains of the influenza virus. Annual flu vaccines protect against the A and B strains that research has predicted to be the most prevalent in the upcoming season.2 However, much like the COVID-19 vaccines, not all influenza vaccines are created equal. Understanding the key differences between the available flu vaccinations can help pharmacists make the most appropriate vaccine recommendations for their patients.2,3
Trivalent Vs Quadrivalent Vaccines
One key difference among vaccine products is determined by the number of viral strains included in the preparation. For example, trivalent vaccines contain 3 strains, including 2 influenza A and 1 influenza B. Quadrivalent vaccines contain 4 strains, including double coverage for both A and B strains.2 Each year, the CDC and the World Health Organization publish recommendations on the composition of strains to be included in the vaccine based on expected widespread presence. The recommended composition of strains for both trivalent and quadrivalent vaccines for the upcoming 2021-2022 season is listed in Table 1.4

Adjuvanted Vaccines
Both trivalent and quadrivalent flu vaccines are available with an adjuvant, which is an ingredient included to create a more robust immune response.2 MF59 is an adjuvant that has been included in the vaccines since 2016,5 and it enhances antigen uptake, increasing migration and activation of immune cells.6 The adjuvanted formulations are approved for individuals 65 years and older.2
Egg-Containing Vs "Egg-Free" Vaccines
Many of the influenza vaccines currently available are produced using egg-based manufacturing. However, newer methods of production have been developed and provide advantages over the traditional method. Currently, there are 3 methods used to produce the different formulations of the influenza vaccine: egg-based manufacturing, cell-based manufacturing, and recombinant technology.7
Most influenza vaccines are produced using egg-based manufacturing. This method can be used to produce live or inactivated influenza vaccines. The egg-based process starts with candidate vaccine viruses (CVVs), which are grown in chicken eggs and provided by the CDC or a partner organization. The CVVs are inserted into fertilized chicken eggs and allowed to replicate for multiple days. After this time, the viral material is collected, killed (if being used for an inactivated vaccine), and purified to produce the viral antigens for the vaccine. Although egg-based manufacturing is the most widely used method, these vaccines often cannot be used in people with egg allergies and can take longer to produce compared with other methods.2 Vaccines grown in eggs are also prone to undergoing egg-adapted changes, which can lead to a less effective vaccine being produced.7,8
As of 2012, the FDA approved the cell-based manufacturing process to be used to produce inactivated influenza vaccines. This process is fairly similar to the egg-based method; however, the CVVs are grown in cells (instead of eggs) and then inserted into cultured mammalian cells to replicate. The viral material is then extracted, killed, and purified for use in the influenza vaccine. Although this method might seem similar to the egg-based method, growing the vaccine in cells allows for faster production of the vaccine material and is not a concern in patients with egg allergies.7 In addition, the cell-based method also avoids the risk of egg-adapted changes.8
The final method of influenza vaccine production involves the use of recombinant technology and was approved for use in 2013. CVVs are not used in this type of production. Instead, the manufacturer utilizes viral DNA to produce hemagglutinin (HA), which is a surface receptor of the influenza virus that functions as an antigen to elicit an immune response. The DNA is then incorporated into a baculovirus (a nonpathogenic virus) to create a recombinant virus. The recombinant virus is then combined with an FDA-approved cell line, where it provides instructions for the cells to produce HA. Once produced, the HA is then purified and used to produce the recombinant influenza vaccine. This method of vaccine production is the fastest currently available and does not require the use of eggs in any part of the process.7 Additionally, since the vaccine material is not grown in eggs, egg-adapted changes are not a concern when utilizing the recombinant method.9
Standard Vs High-Dose Vaccines
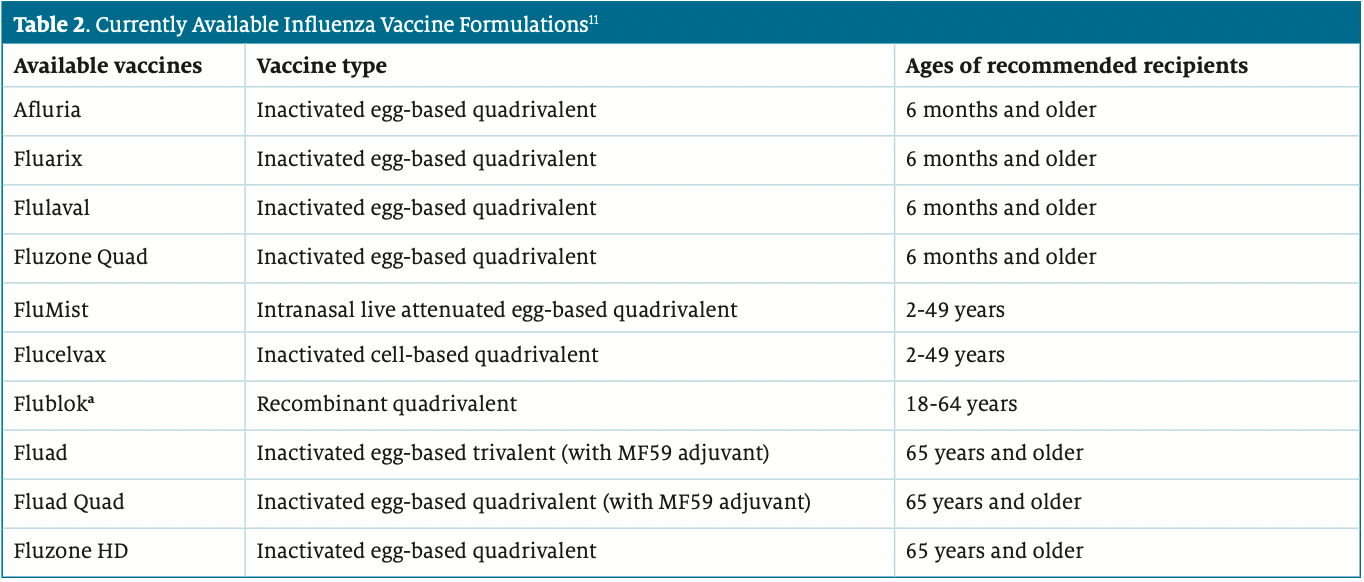
Most influenza formulations are available as a standard dose. However, as of 2009, a more concentrated formulation has been developed as a high-dose option for patients at increased risk of infection (eg, those who are 65 and older). The high-dose formulation contains 4 times the amount of antigen as the standard-dose preparations.10 The high-dose influenza vaccine is only available as a quadrivalent formulation. All currently available influenza vaccine formulations can be found in Table 2.11
Adverse Effects and Contraindications for Flu Vaccines
People who refrained from receiving the COVID-19 vaccine because of evolving safety data might express the same hesitancy toward the upcoming flu vaccines.12 Therefore, it is important to reestablish the safety of vaccinations within the public eye. Adverse effects (AEs) to the annual flu vaccine are typically mild and resolve quickly. Mutual AEs are observed in the inactivated and recombinant vaccines, including soreness, redness, and pain at the injection site, as well as muscle aches, nausea, fever, and headaches.13 According to the results of several studies, injection site pain was found to be more common in quadrivalent doses, which can be attributed to the body’s response to an additional antigen.14 Furthermore, differences in systemic effects have been established between children and adults. Both groups reported headache and malaise; however, children more frequently experienced irritability, whereas fatigue was more common in adults.14
Although live vaccines are associated with more pronounced AEs, a surveillance report of the live attenuated influenza vaccine (LAIV) quadrivalent dose more commonly identified nonserious AEs such as fever, cough, and headache.15 One vaccine, FluMist (AstraZeneca), elicits an immune response by replicating in the epithelial, mucosal cells of the nasopharynx.16 As a result, nasal congestion, rhinorrhea, and sore throat are more commonly reported in people receiving FluMist compared with those getting the inactivated and recombinant vaccines.16
Advisory Committee on Immunization Practices recommendations suggest the LAIV requires greater surveillance of patient characteristics; however, the contraindications of all vaccines should be carefully considered before the administration of any dose.17 All the available vaccines are contraindicated in people with a history of allergic reactions to any component of the vaccine due to the risk of anaphylaxis. Most notably, people with egg allergies should avoid any of the egg-based vaccines listed in Table 2. The LAIV preparation is contraindicated in children aged 2 to 4 years with asthma or wheezing within the past 12 months, concomitant aspirin- or salicylate-containing therapy, immunocompromised for any cause, pregnancy, persons with cochlear implants, and those who have received influenza antiviral medications within the past 48 hours.17
Recommending a Flu Vaccine
The intent of receiving a flu vaccine each year is to prevent severe, life-threatening complications, hospitalizations, and death from the virus.18 Each flu vaccine contains different components and is manufactured in different ways, allowing pharmacists and patients to work together to determine the right vaccine to receive. Two factors to consider when recommending a vaccine for a patient are patient-specific characteristics (eg, age and comorbid conditions) and accuracy of the vaccine with the circulating flu viruses in the community.18 In patients older than 65 or who have weakened immune systems, high-dose or adjuvanted quadrivalent vaccines have demonstrated higher efficacy over standard-dose trivalent vaccines.18 In children, flu vaccine effectiveness has shown to be higher in those who received 2 doses in their first flu season compared with children who received 1 dose.18 Ultimately, receiving a flu vaccine protects the recipient and members of the community, especially more vulnerable populations, from effects of the virus, cardiac events, and worsening of chronic lung disease, and it also reduces hospitalizations in patients with diabetes and chronic lung disease.18
Source:
Stephen Rayborn, PharmD Candidate , C. Michael Gallagher, PharmD Candidate, Lindsey Miller, PharmD Candidate, Jamie L. Wagner, PharmD, BCPS
Supplements, Influenza Guide for Pharmacists July 2021
Pre:How COVID-19 Highlighted Problems with U.S. Food Supply Chain

Send Us A Message
Please leave your message here! We will send detailed technical info and quotation to you!